A 63-year-old man presented to the family medicine clinic with a nonpainful skin lesion on his left forearm. The lesion had grown rapidly since he first noticed it 2 weeks earlier. The patient reported having some purulent and blood-tinged fluid drainage from the lesion. He also experienced several weeks of low-grade fevers, nonproductive cough, and unintentional weight loss. One week earlier, he had been prescribed antibiotics for presumed pneumonia, but his symptoms had not improved since completing treatment. The patient was a farmer in southern Indiana. His medical history was significant only for squamous cell carcinoma of the skin. He had no history of tobacco use.
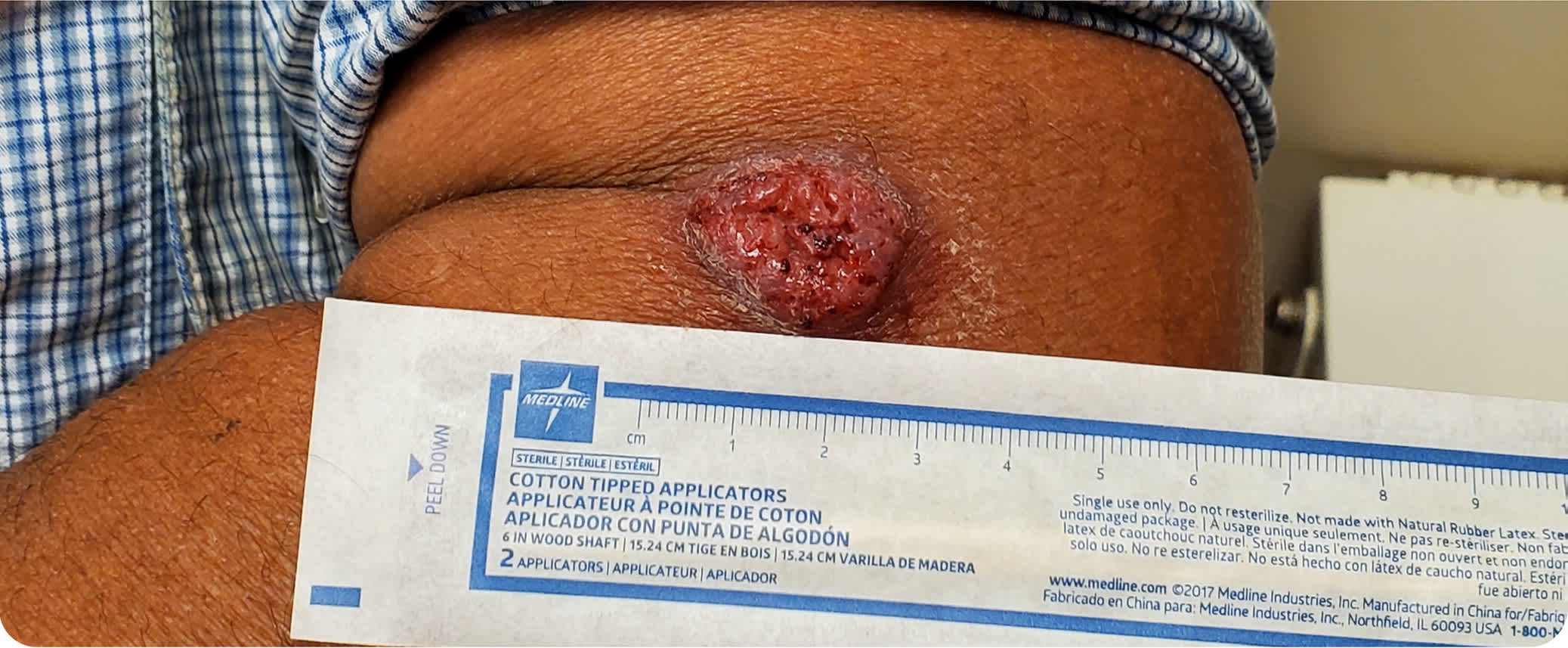
Physical examination revealed a red, verrucous plaque on the lateral aspect of the proximal left forearm. The plaque was firm, raised, nontender, and 2.5 cm in diameter (Figure 1).
FIGURE 1
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
- A. Blastomycosis.
- B. Coccidioidomycosis.
- C. Histoplasmosis.
- D. Pyogenic granuloma.
- E. Verrucous carcinoma.
Discussion
The answer is A: blastomycosis. The condition is caused by inhalation of spores of Blastomyces dermatitidis, a dimorphic fungus. Primary disease occurs in the lungs, but hematogenous spread can affect other areas. The skin is the most commonly involved extrapulmonary organ. In descending order of prevalence, lesions may also be found in the bones, genitourinary system, and central nervous system. Blastomycosis may cause active infection in immunocompetent individuals, unlike histoplasmosis and coccidioidomycosis, which are more common in immunocompromised individuals. B. dermatitidis is endemic to the regions surrounding the Great Lakes, the Ohio and Mississippi River valleys, and the Saint Lawrence River.1
Pulmonary blastomycosis presents similarly to bacterial or viral pneumonia. Common symptoms include cough (often productive), dyspnea, chest pain (sometimes pleuritic), fever, chills, night sweats, and weight loss. Many patients develop pleural effusions. The onset can be insidious, and some patients may be asymptomatic or have a brief, self-limited disease.1,2
Cutaneous blastomycosis usually presents with one or more papules. As they spread, the borders can develop microabscesses. The surfaces can become covered in papillae, giving the lesions a verrucous appearance. These lesions have a similar presentation in individuals of all skin tones.1,3 Diagnosis is confirmed by fungal culture. Microscopic examination of skin scrapings, sputum, or other materials with calcofluor white or potassium hydroxide can show yeast with broad-based buds ranging from 8 to 15 μm in diameter. Urine testing results for Blastomyces antigen may be false positive due to high cross-reactivity with Histoplasma. Chest radiography commonly shows mass-like lesions or alveolar infiltrates.1,4
Mild or moderate cases are treated with oral itraconazole for at least 6 months. Severe cases are managed initially with intravenous amphotericin B until the patient is stabilized, followed by at least 12 months of oral itraconazole. Immunocompromised and pregnant patients, children, and those with central nervous system involvement are typically treated with amphotericin B.1,4
Coccidioidomycosis is caused by the inhalation of spores of the genus Coccidioides, a group of dimorphic fungi endemic to the southwestern United States. Primary infection occurs in the lungs, but it can have cutaneous manifestations such as erythema nodosum and erythema multiforme. Most patients are asymptomatic or minimally symptomatic, but they can present with chest pain, cough, fever, night sweats, and weight loss. The most common sites of dissemination are the skin and soft tissue, genitourinary system, peritoneum, and central nervous system. Disease occurring on the skin can present with a wide array of lesions, including papules, nodules, and ulcerated and verrucous plaques and abscesses.5
Histoplasmosis is caused by the inhalation of spores of Histoplasma capsulatum, a dimorphic fungus commonly found in the Mississippi and Ohio River valleys. Primary infection occurs in the lungs, and hematogenous dissemination affects organs of the reticuloendothelial system. Lesions may form granulomata in the liver and spleen. A small percentage of patients are symptomatic, reporting rheumatologic symptoms or erythema nodosum, a painful, raised, inflammatory lesion of subcutaneous fat usually involving the lower extremities. Exposure leads to asymptomatic disease in most healthy individuals. Clinically evident disseminated disease occurs primarily in individuals with underlying immunosuppression.1,6
Pyogenic granulomata are benign, vascular lesions that develop after minor trauma. They are lobular, friable, and pink to purple in color, depending on the growth phase. The lesions typically grow fast and bleed easily. Pyogenic granulomata are difficult to distinguish from skin cancers and usually require biopsy for a definitive diagnosis. They may occur anywhere on the skin or oral mucosa.7
Verrucous carcinoma is a slow-growing variant of squamous cell carcinoma. It presents as a soft area that is fun-gating and papillomatous. Locations include the skin, oral or genital areas, and the larynx and esophagus. Initially, the lesion may be white. Verrucous carcinoma is not known to metastasize. Lesions in the oral or nasal areas are more common in smokers and those who use oral tobacco products.8
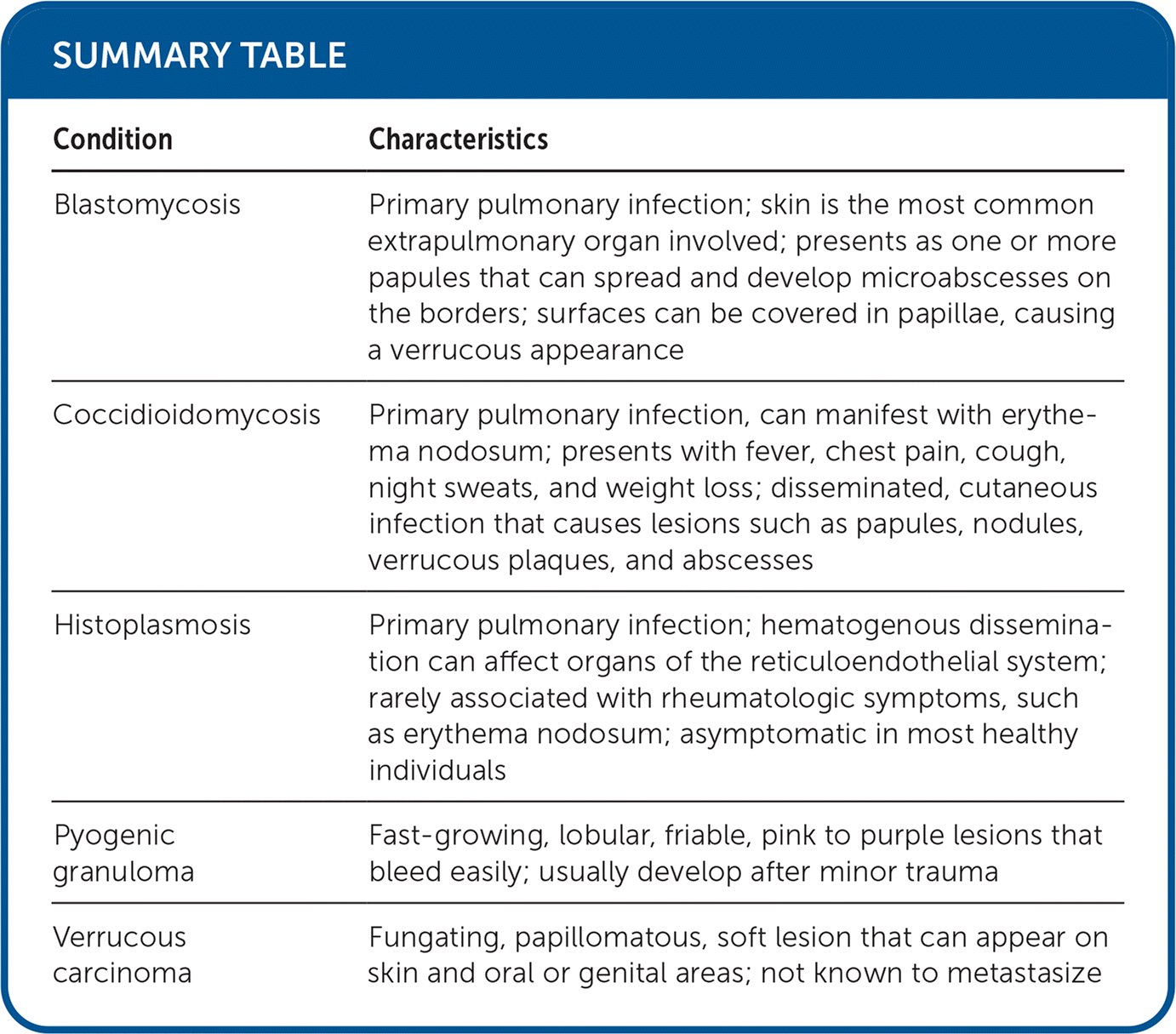
SUMMARY TABLE
| Condition | Characteristics |
|---|---|
| Blastomycosis | Primary pulmonary infection; skin is the most common extrapulmonary organ involved; presents as one or more papules that can spread and develop microabscesses on the borders; surfaces can be covered in papillae, causing a verrucous appearance |
| Coccidioidomycosis | Primary pulmonary infection, can manifest with erythema nodosum; presents with fever, chest pain, cough, night sweats, and weight loss; disseminated, cutaneous infection that causes lesions such as papules, nodules, verrucous plaques, and abscesses |
| Histoplasmosis | Primary pulmonary infection; hematogenous dissemination can affect organs of the reticuloendothelial system; rarely associated with rheumatologic symptoms, such as erythema nodosum; asymptomatic in most healthy individuals |
| Pyogenic granuloma | Fast-growing, lobular, friable, pink to purple lesions that bleed easily; usually develop after minor trauma |
| Verrucous carcinoma | Fungating, papillomatous, soft lesion that can appear on skin and oral or genital areas; not known to metastasize |

